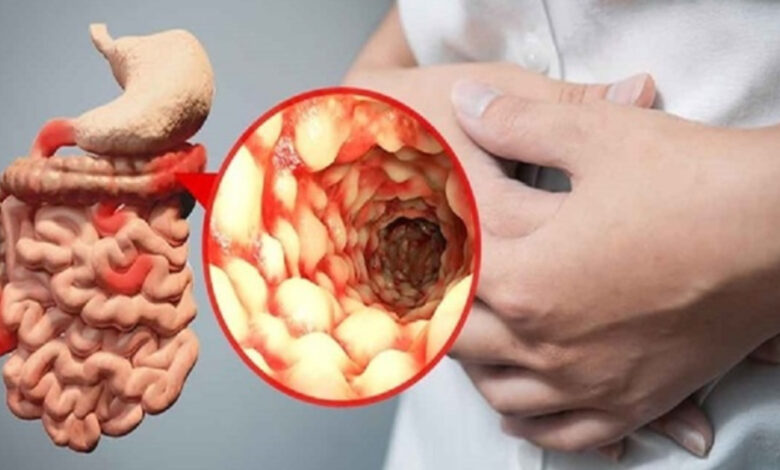
Crohn’s disease is a type of inflammatory bowel disease.
More research about Crohn’s disease is necessary. Researchers aren’t sure how it begins, who is most likely to develop it, or how to best manage it. Despite major treatment advances in the last three decades, no cure is available yet.
Crohn’s disease most commonly occurs in the small intestine and the colon. It can affect any part of your gastrointestinal (GI) tract, from your mouth to your anus. It can involve some parts of the GI tract and skip other parts.
The range of severity for Crohn’s is mild to debilitating. Symptoms vary and can change over time. In severe cases, the disease can lead to life-threatening flares and complications.
Table of Contents
Signs and Symptoms of Crohn’s Disease
Crohn’s disease can affect each patient a little differently. We are here to help guide you through the most common signs and symptoms of Crohn’s disease. The symptoms you or your loved one may experience depends on which part of the GI tract is affected.
Crohn’s is a chronic disease, which means patients will likely experience periods when symptoms are active, known as flares, followed by periods of remission when you may not notice any symptoms at all.
While it is important to recognize the signs of Crohn’s disease, only a doctor can confirm a diagnosis. If you suspect you may have inflammatory bowel diseases (IBD), please schedule an appointment with your doctor to work toward a diagnosis and treatment plan.
GI Tract Inflammation
Crohn’s disease can affect any part of the GI tract, from your mouth to your anus. While symptoms vary from patient to patient, there are some common symptoms of inflammation of the GI tract caused by Crohn’s disease.
-
Persistent diarrhea
-
Rectal bleeding
-
Urgent need to move bowels
-
Abdominal cramps and pain
-
Sensation of incomplete bowel evacuation
-
Constipation, which can lead to bowel obstruction
Crohn’s Disease Complications
While Crohn’s disease is located in the GI tract, it can affect your overall health and cause more serious medical issues.
-
Loss of appetite
-
Weight loss
-
Low energy and fatigue
-
Delayed growth and development in children
In more severe cases, Crohn’s disease can lead to serious complications.
-
Fissures are tears in the lining of the anus, which can cause pain and bleeding especially during bowel movements.
-
A fistula, caused by inflammation, is an abnormal channel that forms between one part of the intestine and another, or between the intestine and the bladder, vagina, or skin. Fistulas are most common in the anal area and require immediate medical attention.
-
A stricture is a narrowing of the intestine as a result of chronic inflammation.
Symptoms Beyond the Intestine
Inflammatory bowel disease (IBD) can cause systemic symptoms outside the GI tract that affect your overall health and your quality of life.
-
Redness or pain in the eyes, or vision changes
-
Mouth sores
-
Swollen and painful joints
-
Skin complications, such as bumps, sores, or rashes
-
Fever
-
Loss of appetite
-
Weight Loss
-
Fatigue
-
Night sweats
-
Loss of normal menstrual cycle
-
Osteoporosis
-
Kidney stones
-
Rare liver complications, including primary sclerosing cholangitis and cirrhosis
Causes
The exact cause of Crohn’s disease is unclear, but it is thought to stem from an abnormal reaction in the immune system.
The theory is that the immune system attacks foods, good bacteria, and beneficial substances as if they are unwanted substances.
During the attack, white blood cells build up in the lining of the gut, and this buildup triggers inflammation. The inflammation leads to ulcerations and bowel injury.
However, it is unclear whether the abnormal immune system causes Crohn’s disease or results from it.
Factors that may increase the risk of inflammation include:
- genetic factors
- the individual’s immune system
- environmental factors
Around 3 in 20 people with Crohn’s have a close relative with the condition. If an identical twin has Crohn’s disease, the other twin has a 70 percent chance of having it, too.
A bacterium or virus may play a role. E. coli bacteria has been linked to Crohn’s disease, for instance.
Smoking is another risk factor.
Treatment
Treatment may involve medication, surgery, and nutritional supplements.
The aim is to control inflammation, correct nutritional problems, and relieve symptoms.
There is no cure for Crohn’s disease, but some treatments can help by reducing the number of times a patient experiences recurrences.
Crohn’s disease treatment depends on:
- where the inflammation is situated
- the severity of the disease
- complications
- the patient’s response to previous treatment for recurring symptoms
Some people can have long periods, even years, without any symptoms. This is known as remission. However, there will usually be recurrences.
As periods of remission vary so much, it can be hard to know how effective treatment has been. It is impossible to predict how long a period of remission is going to be.
Medication for Crohn’s disease
- Anti-inflammation drugs – the doctor will most likely start with mesalamine (Sulfasalazine), which helps control inflammation.
- Cortisone or steroids – corticosteroids are drugs containing cortisone and steroids.
- Antibiotics – fistulas, strictures, or prior surgery may cause bacterial overgrowth. Doctors will generally treat this by prescribing ampicillin, sulfonamide, cephalosporin, tetracycline, or metronidazole.
- Anti-diarrheal and fluid replacements – when the inflammation subsides, diarrhea usually becomes less of a problem. However, sometimes the patient may need something for diarrhea and abdominal pain.
Biologics
Biologics are a new type of drug that scientists have developed from a living organism. They reduce the body’s immune response by targeting proteins that lead to inflammation.
Biologics appear to help people with Crohn’s disease.
Examples of biologics for Crohn’s include:
- infliximab (Remicade)
- adalimumab (Humira)
- 6-mercaptopurine (Purinethol)
- methotrexate
- imuran (Azathioprine)
- certolizumab pegol (Cimzia)
Biologic treatments can have side effects, include vomiting, nausea, and a weaker resistance to infection.
Some studies suggest that the use of biologics can reduce the chance that a person will need abdominal surgery within 10 years to 30 percent. Before the introduction of biologics, researchers put this figure at 40–55 percent.
Biologics also appear to reduce the risk of adverse effects that can arise when a person uses corticosteroids.
There are different types of biologic drugs, and individuals react differently to them. A doctor will recommend a suitable option, and they may suggest trying an alternative or a combination of drugs if the first one does not work.
Surgery
The majority of Crohn’s disease patients may need surgery at some point. When medications no longer control symptoms, the only solution is to operate. Surgery can relieve symptoms that did not respond to medication, or to correct complications, such as abscess, perforation, bleeding, and blockage.
Removing part of the intestine can help, but it does not cure Crohn’s disease. Inflammation often returns to the area next to where the affected part of the gut was removed. Some Crohn’s disease patients may require more than one operation during their lives.
In some cases, a colectomy is needed, in which the whole colon is removed. The surgeon will make a small opening in front of the abdominal wall, and the tip of the ileum is brought to the skin’s surface to form an opening called a stoma. Feces exit the body through the stoma. A pouch collects the feces. Doctors say that a patient who has a stoma can carry on leading a normal and active life.
If the surgeon can remove the diseased section of the intestine and then connect the intestine again, no stoma is needed.
The patient and their doctor need to consider surgery very carefully. It is not appropriate for everyone. The patient has to bear in mind that after the operation, the disease will recur.
Most people with Crohn’s disease can live normal and active lives, hold jobs, raise families, and function successfully.
For any important information please contact us Email GadgetsNg info@gadgetsng.com
[Button id="1"]



Online medicine order https://indiaph24.store/# buy prescription drugs from india
cheapest online pharmacy india