Table of Contents
What is psoriasis?
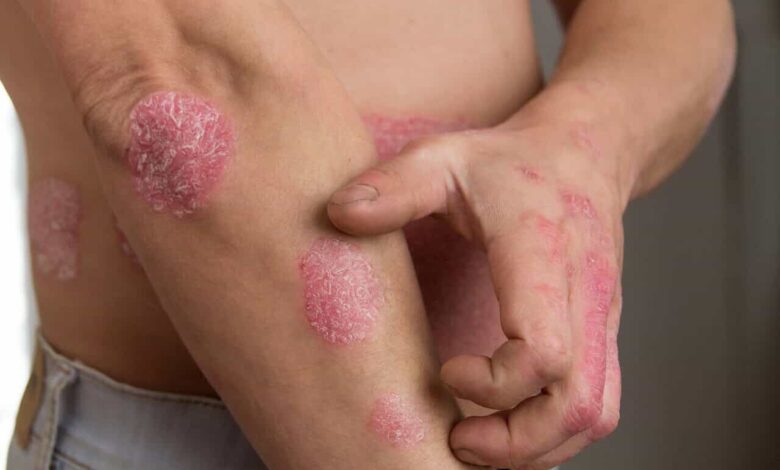
Psoriasis is a noncontagious, chronic skin disease that produces plaques of thickened, scaly skin. The dry flakes of silvery-white skin scales result from the excessively rapid proliferation of skin cells. Psoriasis is fundamentally a defective inflammatory response.
The proliferation of skin cells is triggered by inflammatory chemicals produced by specialized white blood cells called T-cells. Psoriasis commonly affects the skin of the elbows, knees, and scalp.
The spectrum of this disease ranges from mild with limited involvement of small areas of skin to severe psoriasis with large, thick plaques to red inflamed skin affecting the entire body surface.
Psoriasis is considered an incurable, long-term (chronic) inflammatory skin condition. It has a variable course, periodically improving and worsening. It is not unusual for psoriasis to spontaneously clear for years and stay in remission. Many people note a worsening of their symptoms in the colder winter months.
Psoriasis affects all races and both sexes. Although psoriasis can be seen in people of any age, from babies to seniors, most commonly patients are first diagnosed in their early adult years. The self-esteem and quality of life of patients with psoriasis is often diminished because of the appearance of their skin.
Recently, it has become clear that people with psoriasis are more likely to have diabetes, high blood lipids, cardiovascular disease, and a variety of other inflammatory diseases. This may reflect an inability to control inflammation. Caring for psoriasis takes medical teamwork.
Types
There are several forms of psoriasis, as described below.
Plaque psoriasis
About 80–90% of people with psoriasis have plaque psoriasis. It usually shows as raised, inflamed, red lesions, covered by silvery, white scales, most often on the elbows, knees, scalp, and lower back.
Inverse psoriasis
Inverse psoriasis develops in the following areas:
- the armpits
- the groin
- under the breasts
- other skin folds, such as around the genitals and buttocks
Inverse psoriasis has red lesions, usually without the scales that occur in plaque psoriasis. The lesions might be smooth and shiny.
Irritation from rubbing and sweating can make this type of psoriasis worse due to its location in skin folds and tender areas. It is more common in people who are overweight and those with deep skin folds.
Erythrodermic psoriasis
Erythrodermic psoriasis is a particularly inflammatory but rare type that can cause large areas of fiery redness across the surface of the body.
People with unstable plaque psoriasis, where lesions do not have clearly defined edges, may develop erythrodermic psoriasis. There may also be exfoliation, or peeling of the skin, severe itching, and pain.
Erythrodermic psoriasis disrupts the body’s chemical balance. This interference may cause protein and fluid loss that can lead to severe illness.
Edema, or swelling from fluid retention, may also occur. This complication is likely to develop around the ankles. The body may have difficulty regulating its temperature, which can cause shivering.
Erythrodermic psoriasis can also lead to pneumonia and congestive heart failure.
The complications of erythrodermic psoriasis can be dangerous. Anyone who shows symptoms of this condition should see a doctor right away.
People with erythrodermic psoriasis may spend time in the hospital if symptoms are severe.
Guttate psoriasis
Guttate psoriasis often starts in childhood or young adulthood. It appears as small, red, individual spots on the skin. The spots are not usually as thick or as crusty as the lesions in plaque psoriasis.
A range of conditions can trigger guttate psoriasis, including:
- upper respiratory infections
- streptococcal infections
- tonsillitis
- stress
- injury to the skin
- certain medications, including anti-malarials, lithium, and beta-blockers.
Guttate psoriasis may resolve without treatment and never return. However, it may clear and reappear later as patches of plaque psoriasis.
Pustular psoriasis
Pustular psoriasis affects adults more than children, and it accounts for fewer than 5% of psoriasis cases.
It appears as white pustules, or blisters of noninfectious pus, which red skin surrounds. It can affect certain areas of the body, for example, the hands and feet, or most of the body. It is not an infection, and it is not contagious.
Pustular psoriasis tends to have a cycle, in which the formation of pustules and scaling follows reddening of the skin.
While psoriasis can form anywhere on the human body, below are some of the most common areas.
Causes
While the cause of psoriasis is still unclear, scientists believe that it is an autoimmune disease.
Autoimmune diseases affect the immune system, which produces T cells to protect the body against infectious agents.
In people with psoriasis, triggers can lead to their genes instructing the immune system to target the wrong cells. T cells respond to a trigger as if they are fighting an infection or healing a wound. They produce chemicals that cause inflammation.
In psoriasis, this autoimmune activity leads to the excessive growth of skin cells. Typically, skin cells take about 21–28 days to replace themselves. However, in people with psoriasis, they take around 2–6 days.
Triggers will be different in each individual with psoriasis, but common triggers include:
- stress and anxiety
- injuries to the skin
- infections
- hormonal changes
Medications that can trigger a psoriasis flare include:
- lithium
- anti-malarials
- quinidine
- indomethacin
Some people associate psoriasis with allergies, diet, and weather, but no evidence has yet supported these theories.
Importantly, psoriasis is not contagious. Knowing this can help people with the disease cope with the more challenging parts of socializing.
Oral and Injectable Medications for Psoriasis
When other treatments fail, some doctors prescribe oral or injectable drugs to treat psoriasis. Some of these medications affect the immune system.
- Methotrexate.
This medication is also used as a chemotherapy drug for cancer and for various forms of arthritis. It can dramatically clear up psoriasis lesions. However, it can cause side effects, so your doctor will have you come in for regular blood tests.
- Oral retinoids.
These compounds with vitamin-A-like properties can be mildly helpful to people with severe psoriasis. Women of childbearing age need to use birth control with this medication because it is linked with an increased risk for birth defects.
- Biologics.
These medications control your body’s immune response. They’re often used to treat severe psoriasis and psoriatic arthritis. These drugs, which are made from human or animal proteins, are quite effective but extremely expensive. They include adalimumab (Humira), brodalumab (Siliq), certolizumab pegol (Cimzia), etanercept (Enbrel), guselkumab (Tremfya), infliximab (Inflectra, Remicade, Renflexis), ixekizumab (Taltz), risankizumab-rzaa(SKYRIZI),secukinumab (Cosentyx), tildrakizumab (Ilumya), and ustekinumab (Stelara). Another drug, apremilast (Otezla), has been found to be effective in reducing joint pain and psoriatic skin symptoms. It works by suppressing an enzyme involved in inflammation.
Natural Psoriasis Treatments
If medications fail to relieve the symptoms of psoriasis or cause unwanted side effects, people may try natural remedies, such as herbs and vitamins, for relief. Some people with psoriasis find natural sunlight and ocean water helpful. Some seaside resorts offer special programs for people with psoriasis.
If you are considering natural remedies for psoriasis, here’s what you should know about some of the more commonly used remedies:
- Dead Sea salts. Bath solutions, such as Dead Sea salts, oil, oilated oatmeal, or Epsom salts can help psoriasis by removing scales and easing itching. To try Dead Sea salts and other bath solutions, mix them in the bath as directed, then soak in the tub for about 15 minutes. As soon as you get out of the tub, apply a moisturizer to the skin. Don’t expect a lot of improvement, however.
- Aloe vera. Preliminary research suggests that topical cream from the aloe vera plant may improve symptoms of psoriasis. One study showed that topical aloe vera was more effective than placebo. This product is of only minimal benefit, at best.
- Fish oil. Fish oil may be helpful for psoriasis when taken as an injection by vein, but it doesn’t seem to have a positive effect when taken by mouth. However, some research showed that it might give added benefit to UVB light therapy.
- Cayenne. Cayenne peppers have been used medicinally for thousands of years. Capsaicin, the ingredient in peppers that gives them their heat, is also the active ingredient in many pain-relieving gels and creams. In one study, applying capsaicin cream to the skin relieved itching and skin lesions in people with psoriasis. Capsaicin can cause a burning sensation to the skin, which improves the longer you use it. It’s important to wash your hands immediately after rubbing in capsaicin and not touch your eyes or mouth while you have capsaicin on your hands.
- Diet. Obese psoriasis patients who lose weight report significant improvement in their symptoms, some research has shown. Evidence is lacking that other dietary restrictions such as gluten-free make any difference in the symptoms of psoriasis.
For any important information please contact us Email GadgetsNg info@gadgetsng.com
[Button id="1"]



pharmacy website india https://indiaph24.store/# pharmacy website india
indian pharmacies safe