Prevention Of fibromyalgia (fatigue, sleep, memory and mood issues)
Fibromyalgia Health Center
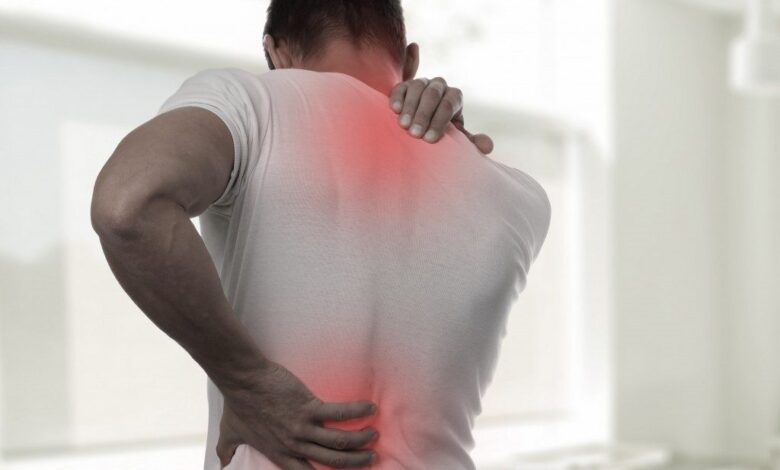
Table of Contents
What is fibromyalgia?
Fibromyalgia is a long-term (chronic) condition.
It causes:
- pain in the muscles and bones (musculoskeletal pain)
- areas of tenderness
- general fatigue
- sleep and cognitive disturbances
This condition can be hard to understand, even for healthcare providers. Its symptoms mimic those of other conditions, and there aren’t any real tests to confirm the diagnosis. As a result, fibromyalgia is often misdiagnosed.
In the past, some healthcare providers even questioned whether fibromyalgia was real. Today, it is much better understood. Some of the stigma that used to surround it has eased.
Fibromyalgia can still be challenging to treat. But medications, therapy, and lifestyle changes can help you to manage your symptoms and to improve your quality of life.
Fibromyalgia symptoms
Fibromyalgia causes what’s now referred to as “regions of pain.” Some of these regions overlap with what was previously referred to as areas of tenderness called “trigger points” or “tender points.” However, some of these previously noted areas of tenderness have been excluded.
The pain in these regions feels like a consistent dull ache. Your healthcare provider will consider a diagnosis of fibromyalgia if you’ve experienced musculoskeletal pain in 4 out of the 5 regions of pain outlined in the 2016 revisions to the fibromyalgia diagnostic criteria.
This diagnostic protocol is referred to as “multisite pain.” It’s in contrast to the 1990 fibromyalgia diagnostic criteria definition for “chronic widespread pain.”
This process of diagnosis focuses on the areas of musculoskeletal pain and severity of pain as opposed to an emphasis on pain duration, which was the previously the focal criteria for a fibromyalgia diagnosis.
Other symptoms of fibromyalgia include:
- fatigue
- trouble sleeping
- sleeping for long periods of time without feeling rested (nonrestorative sleep)
- headaches
- depression
- anxiety
- trouble focusing or paying attention
- pain or a dull ache in the lower belly
- dry eyes
- bladder problems, such as interstitial cystitis
In people with fibromyalgia, the brain and nerves may misinterpret or overreact to normal pain signals. This may be due to a chemical imbalance in the brain or abnormality in the dorsal root ganglion affecting central pain (brain) sensitization.
Fibromyalgia can also affect your emotions and energy level.
Fibromyalgia fog | Fog
Fibromyalgia fog also known as “fibro fog” or “brain fog” is a term some people use to describe the fuzzy feeling they get. Signs of fibro fog include:
- memory lapses
- difficulty concentrating
- trouble staying alert
Some people find mental fogginess from fibromyalgia more upsetting than pain.
Fibromyalgia symptoms in women | Symptoms in women
Fibromyalgia symptoms have generally been more severe in women than in men. Women have more widespread pain, IBS symptoms, and morning fatigue than men. Painful periods are also common.
However, when the 2016 revisions to the diagnostic criteria are applied, more men are being diagnosed with fibromyalgia, which may reduce the degree of distinction between the pain levels men and women experience. More research needs to be done to further evaluate that distinction.
The transition to menopause could make fibromyalgia worse.
Complicating things is the fact that some symptoms of menopause and fibromyalgia look almost identical.
Fibromyalgia in me
Men also get fibromyalgia. Yet, they may remain undiagnosed because this is seen as a woman’s disease. However, current statistics show that as the 2016 diagnostic protocol is more readily applied, more men are being diagnosed.
Men also have severe pain and emotional symptoms from fibromyalgia. The condition affects their quality of life, career, and relationships.
Part of the stigma and difficulty in getting diagnosed stems from society’s expectation that men who are in pain should “suck it up.”
Fibromyalgia trigger points
In the past, people were diagnosed with fibromyalgia if they had widespread pain and tenderness in at least 11 out of 18 specific trigger points around their body. Healthcare providers would check to see how many of these points were painful by pressing firmly on them.
Common trigger points included the:
- back of the head
- tops of the shoulders
- upper chest
- hips
- knees
- outer elbows
For the most part, trigger points are no longer a part of the diagnostic process.
Instead, healthcare providers may diagnose fibromyalgia if you’ve had pain in 4 out of the 5 areas of pain as defined by the 2016 revised diagnostic criteria, and you have no other diagnosable medical condition that could explain the pain.
Fibromyalgia pain
Pain is the hallmark fibromyalgia symptom. You’ll feel it in various muscles and other soft tissues around your body.
The pain can range from a mild achiness to an intense and almost unbearable discomfort. Its severity could dictate how well you cope day to day.
Fibromyalgia appears to stem from an abnormal nervous system response. Your body overreacts to things that shouldn’t normally be painful. And you may feel the pain in more than one area of your body.
However, available research still doesn’t pinpoint an exact cause for fibromyalgia. Research continues to evolve in better understanding this condition and its origin.
Chest pain
When fibromyalgia pain is in your chest, it can feel frighteningly similar to the pain of a heart attack.
Chest pain in fibromyalgia is actually centered in the cartilage that connects your ribs to your breastbone. The pain may radiate to your shoulders and arms.
Fibromyalgia chest pain may feel:
- sharp
- stabbing
- like a burning sensation
And similar to a heart attack, it can make you struggle to catch your breath.
Back pain
Your back is one of the most common places to feel pain. About 80 percent of Americans have low back pain at some point in their lives. If your back hurts, it may not be clear whether fibromyalgia is to blame, or another condition like arthritis or a pulled muscle.
Other symptoms like brain fog and fatigue can help pinpoint fibromyalgia as the cause. It’s also possible to have a combination of fibromyalgia and arthritis.
The same medications you take to relieve your other fibromyalgia symptoms can also help with back pain. Stretching and strengthening exercises can help provide support to the muscles and other soft tissues of your back.
Leg pain
You can also feel fibromyalgia pain in the muscles and soft tissues of your legs. Leg pain can feel similar to the soreness of a pulled muscle or the stiffness of arthritis. It can be:
- deep
- burning
- throbbing
Sometimes fibromyalgia in the legs feels like numbness or tingling. You may have a creepy crawling sensation. An uncontrollable urge to move your legs is a sign of restless legs syndrome (RLS), which can overlap with fibromyalgia.
Fatigue sometimes manifests in the legs. Your limbs can feel heavy, as if they’re held down by weights.
Causes
Doctors aren’t sure what causes it, but some think it’s a problem with how your brain and spinal cord process pain signals from your nerves.
We do know certain things suggest you’re more likely to get it:
- You’re a woman.
- You have another painful disease, such as arthritis, or an infection.
- You have a mood disorder, like anxiety or depression.
- You were physically or emotionally abused or have PTSD.
- You rarely exercise.
- Other family members have it.
Treatment
Medical attention is needed because fibromyalgia can be difficult to manage. As it is a syndrome, each patient will experience a different set of symptoms, and an individual treatment plan will be necessary.
Treatment may include some or all of the following:
- an active exercise program
- acupuncture
- psychotherapy
- behavior modification therapy
- chiropractic care
- massage
- physical therapy
- low-dose anti-depressants, although these are not a first-line treatment
People with fibromyalgia need to work with their doctor to come up with a treatment plan that provides the best results.
Drugs
Drugs may be recommended to treat certain symptoms.
These may include over-the-counter (OTC) pain relievers. However, the European League Against Rheumatism (EULAR) issued a recommendation against using non-steroidal anti-inflammatory drugs (NSAIDs) to treat fibromyalgia in their updated 2016 guidelines.
Antidepressants, such as duloxetine, or Cymbalta, and milnacipran, or Savella, may help reduce pain. Anti-seizure drugs, such as gabapentin also known as Neurontin, and pregabalin, or Lyrica, may be prescribed.
However, a review has suggested that patients often stop using these drugs because they are not effective in relieving pain or because of their adverse effects.
Patients should tell the doctor about any other medications they are taking to avoid side-effects and interactions with other drugs.
Exercise
A combination of aerobic exercise and resistance training, or strength training, has been linked to a reduction in pain, tenderness, stiffness, and sleep disturbance, in some patients.
If exercise is helping with symptoms, it is important to maintain consistency in order to see progress. Working out with a partner or personal trainer may help to keep the exercise program active.
Acupuncture
Some patients have experienced improvements in their quality of life after starting acupuncture therapy for fibromyalgia. The number of sessions required will depend on the symptoms and their severity.
One study found that 1 in 5 people with fibromyalgia use acupuncture within 2 years of diagnosis. The researchers concluded that it may improve pain and stiffness. However, they call for more studies.
Behavior modification therapy
Behavior modification therapy is a form of cognitive behavioral therapy (CBT) that aims to reduce negative, stress- or pain-increasing behaviors and improve positive, mindful behaviors. It includes learning new coping skills and relaxation exercises.
Causes
The exact cause of fibromyalgia is unclear. However, current thinking in the field of Rheumatology suggests that fibromyalgia is a problem with central pain processing in the brain, where there may be an increased sensitivity or perception of pain to a given trigger.
There is a range of likely risk factors, including:
- a stressful, traumatic physical or emotional event, such as a car accident
- repetitive injuries
- rheumatoid arthritis or other autoimmune diseases, such as lupus
- central nervous system (CNS) problems
- the way our genes regulate how we process painful stimuli
Fibromyalgia may also be hereditary. Females who have a close relative with fibromyalgia have a higher risk of experiencing it themselves.
People with rheumatoid arthritis, lupus, or spinal arthritis, known ankylosing spondylitis, have a higher risk of developing fibromyalgia, as do patients with some other rheumatic diseases.
For any important information please contact us Email GadgetsNg info@gadgetsng.com
[Button id="1"]



Your mode of explaining the whole thing in this post is actually good, every one be capable of
without difficulty be aware of it, Thanks a lot.
It is in point of fact a great and useful piece of information.
I’m happy that you just shared this useful info with us.
Please keep us informed like this. Thank you for sharing.
Hey would you mind letting me know which webhost you’re using?
I’ve loaded your blog in 3 completely different internet
browsers and I must say this blog loads a lot faster then most.
Can you suggest a good hosting provider at a honest price?
Cheers, I appreciate it!
No matter if some one searches for his required thing, thus he/she wishes to be available that in detail,
thus that thing is maintained over here.
I have learn some just right stuff here. Definitely value bookmarking for revisiting.
I surprise how much attempt you place to make this sort of wonderful informative website.
I all the time used to read piece of writing in news papers but now as I am a user of internet thus from now I am using net for
articles or reviews, thanks to web.
I really like what you guys are up too. Such clever work and reporting!
Keep up the superb works guys I’ve included you guys to blogroll.
I am curious to find out what blog system you have been working with?
I’m having some small security issues with my latest website and I would like to find something more risk-free.
Do you have any solutions?
This piece of writing will assist the internet users
for building up new website or even a weblog from start to end.
Woah! I’m really enjoying the template/theme of this blog.
It’s simple, yet effective. A lot of times it’s tough to get
that “perfect balance” between superb usability and appearance.
I must say you have done a amazing job with this.
In addition, the blog loads extremely quick for me on Firefox.
Excellent Blog!
Have you ever considered about including a little bit more than just your articles?
I mean, what you say is valuable and all. But just imagine if you added
some great photos or video clips to give your posts more, “pop”!
Your content is excellent but with pics and videos, this blog
could certainly be one of the best in its niche.
Awesome blog!
Excellent blog here! Also your site loads up very fast!
What web host are you using? Can I get your affiliate
link to your host? I wish my web site loaded up as fast as yours lol
Hi there, just became aware of your blog through Google, and found that it’s really informative.
I am gonna watch out for brussels. I will be grateful if you continue this in future.
Numerous people will be benefited from your writing.
Cheers!
Hi! Do you use Twitter? I’d like to follow you if that would be okay.
I’m absolutely enjoying your blog and look forward to new updates.
I’m not that much of a online reader to be honest but your sites really nice, keep it up!
I’ll go ahead and bookmark your website to come back down the road.
Cheers
Amazing things here. I am very satisfied to see your post.
Thank you so much and I am looking ahead to contact you. Will you kindly drop me a e-mail?
When some one searches for his required thing, therefore he/she
needs to be available that in detail, thus that
thing is maintained over here.
With havin so much content do you ever run into any issues of plagorism or copyright
infringement? My blog has a lot of completely unique content I’ve either created myself or outsourced but it looks
like a lot of it is popping it up all over the internet
without my permission. Do you know any solutions to help protect against content from being ripped off?
I’d certainly appreciate it.
Wow, fantastic blog layout! How long have you been blogging for?
you make blogging look easy. The overall look of your web site
is great, as well as the content!
Hi there, I do think your site might be having
browser compatibility issues. Whenever I look at your
web site in Safari, it looks fine but when opening in I.E., it has some overlapping issues.
I just wanted to provide you with a quick heads up! Aside from that, wonderful site!
We stumbled over here different website and thought I should check things out.
I like what I see so now i am following you. Look forward to looking at
your web page yet again.
Hi there, just wanted to say, I loved this post.
It was practical. Keep on posting!
Great blog right here! Additionally your site loads up fast!
What host are you the use of? Can I am getting your affiliate hyperlink to your host?
I desire my website loaded up as quickly as yours lol
Heya i’m for the first time here. I came across this board and I find
It truly useful & it helped me out much. I hope to give something back
and aid others like you helped me.
It’s going to be ending of mine day, except before
ending I am reading this great piece of writing to increase my know-how.
Hi i am kavin, its my first time to commenting anyplace, when i read this paragraph i thought i could also make comment due to this brilliant piece of writing.
What’s Happening i am new to this, I stumbled upon this I have discovered It absolutely useful and it has aided me
out loads. I hope to contribute & aid different users like its helped me.
Great job.
Excellent site. Lots of useful information here. I’m sending it
to a few buddies ans also sharing in delicious. And certainly, thank you in your
effort!
Hey! I could have sworn I’ve been to this blog before but after checking through some of the post I realized it’s new to me.
Anyways, I’m definitely happy I found it and I’ll be book-marking and checking back often!
Hi, for all time i used to check webpage posts here in the early hours in the morning, since
i enjoy to learn more and more.
If you want to get a good deal from this article then you have to apply these strategies to your won blog.
Its like you read my mind! You appear to know a lot about
this, like you wrote the book in it or something. I think that you can do with a few pics to drive the message home a bit, but instead
of that, this is wonderful blog. An excellent read.
I’ll definitely be back.
What’s up mates, how is everything, and what you want to
say regarding this article, in my view its genuinely remarkable
in favor of me.
It’s amazing to pay a quick visit this web site and reading the views
of all mates regarding this article, while I am also zealous of getting experience.
We are a group of volunteers and opening a brand new scheme in our community.
Your site offered us with useful info to work on. You have done
a formidable activity and our whole neighborhood
will likely be grateful to you.
Fine way of explaining, and pleasant paragraph to take information regarding my presentation focus,
which i am going to deliver in college.
I have read so many articles regarding the blogger lovers
however this post is really a nice piece
of writing, keep it up.
Hello! I understand this is somewhat off-topic however I had to ask.
Does building a well-established blog like yours require a massive amount work?
I’m completely new to writing a blog but I do write in my
journal daily. I’d like to start a blog so I can share my
own experience and feelings online. Please let me know if you
have any kind of ideas or tips for new aspiring bloggers.
Thankyou!
What’s up, its pleasant post about media print, we all know media is a
impressive source of information.
Way cool! Some extremely valid points! I appreciate you penning
this write-up plus the rest of the website is also very
good.
Hello would you mind stating which blog platform you’re using?
I’m going to start my own blog in the near future
but I’m having a difficult time selecting between BlogEngine/Wordpress/B2evolution and Drupal.
The reason I ask is because your layout seems different
then most blogs and I’m looking for something completely unique.
P.S Apologies for getting off-topic but I had to ask!
It’s an amazing article for all the web people; they will get benefit from it I am
sure.
Hurrah! At last I got a web site from where I be capable of in fact get useful facts regarding my study and
knowledge.
Very descriptive blog, I loved that bit. Will there be a part 2?
always i used to read smaller posts that
also clear their motive, and that is also happening with this piece
of writing which I am reading at this place.
This is my first time pay a visit at here and i am in fact impressed
to read everthing at one place.
Write more, thats all I have to say. Literally, it seems
as though you relied on the video to make your point. You obviously know what youre talking about,
why waste your intelligence on just posting videos to your weblog when you
could be giving us something informative to read?
Hi! Would you mind if I share your blog with my twitter group?
There’s a lot of people that I think would really appreciate your content.
Please let me know. Thank you
Verify out our recommended slots to play
in 2023 section to make the appropriate decisuon for
you.
Feel free to surf to my web page :: 바카라사이트
I just like the helpful information you supply on your articles.
I will bookmark your weblog and test once more right here regularly.
I’m reasonably sure I will be told plenty of new stuff right here!
Good luck for the next!
Hi, just wanted to tell you, I loved this blog post. It was helpful.
Keep on posting!
Wow! After all I got a website from where I know how to in fact
get useful information regarding my study and knowledge.
It’s awesome to pay a visit this website and reading the views of all mates regarding this post, while
I am also zealous of getting experience.
If you are going for best contents like myself, only visit this web
page all the time since it offers feature contents,
thanks
Wow that was strange. I just wrote an really long comment
but after I clicked submit my comment didn’t appear.
Grrrr… well I’m not writing all that over again. Anyhow, just wanted to say great blog!
Nice blog here! Also your website loads up very fast!
What host are you using? Can I get your affiliate link to
your host? I wish my site loaded up as fast as yours lol
When I originally commented I clicked the “Notify me when new comments are added” checkbox
and now each time a comment is added I get four e-mails with the
same comment. Is there any way you can remove me from that
service? Many thanks!
Hi, i think that i saw you visited my web site so i came to “return the favor”.I am attempting to find things to enhance my site!I suppose its ok to use some of
your ideas!!
Very good blog post. I absolutely love this site. Continue the good work!
Awesome blog! Do you have any suggestions for aspiring writers?
I’m planning to start my own website soon but I’m a little
lost on everything. Would you propose starting with a free platform
like WordPress or go for a paid option? There are so many options out there that I’m totally confused ..
Any recommendations? Kudos!
It’s an remarkable paragraph designed for all the web people; they will obtain advantage from it I am sure.
Its like you read my mind! You appear to know a lot about this, like you wrote the book in it or something.
I think that you could do with a few pics to drive the message home a little bit, but other than that, this is magnificent blog.
A fantastic read. I will definitely be back.
Excellent goods from you, man. I have understand
your stuff previous to and you’re just extremely fantastic.
I really like what you have acquired here, really like what you are stating and the way in which you say it.
You make it enjoyable and you still care for to keep it sensible.
I cant wait to read much more from you. This is actually a terrific
website.
Thanks very nice blog!
Genuinely when someone doesn’t know afterward its up to other viewers
that they will help, so here it takes place.
Just desire to say your article is as surprising. The clearness in your post is
simply spectacular and i could assume you’re an expert
on this subject. Fine with your permission allow me to grab your RSS feed to keep updated with forthcoming post.
Thanks a million and please continue the rewarding work.
Hi there, I read your blogs on a regular basis.
Your story-telling style is awesome, keep it up!
Very great post. I simply stumbled upon your weblog
and wanted to say that I have truly enjoyed browsing your
blog posts. In any case I will be subscribing for your feed and I hope you write again soon!
Woah! I’m really digging the template/theme of this website.
It’s simple, yet effective. A lot of times it’s difficult to get that “perfect balance” between user friendliness
and appearance. I must say that you’ve done a amazing job with this.
In addition, the blog loads super quick for me on Internet explorer.
Superb Blog!
We are a group of volunteers and starting a brand new
scheme in our community. Your website provided us with useful information to work on. You have performed
an impressive activity and our entire community will probably be thankful to you.
Wonderful blog! I found it while surfing around on Yahoo News.
Do you have any suggestions on how to get listed in Yahoo News?
I’ve been trying for a while but I never seem to
get there! Thank you
Usually I don’t learn post on blogs, however I would like
to say that this write-up very forced me to
check out and do it! Your writing taste has been amazed me.
Thanks, very nice article.
Actually no matter if someone doesn’t know afterward its up to
other people that they will assist, so here it takes place.
I’m curious to find out what blog system you happen to be using?
I’m experiencing some minor security issues with
my latest blog and I would like to find something more safeguarded.
Do you have any solutions?
What a material of un-ambiguity and preserveness of valuable familiarity concerning
unpredicted feelings.
Thank you for the auspicious writeup. It in fact was a
amusement account it. Look advanced to far added agreeable from you!
However, how can we communicate?
Very good blog! Do you have any helpful hints for aspiring writers?
I’m hoping to start my own blog soon but I’m a little lost on everything.
Would you propose starting with a free platform like WordPress or go for a paid option? There are
so many options out there that I’m completely confused ..
Any suggestions? Thanks a lot!
Great article, totally what I needed.
I am now not certain where you are getting your info, however
great topic. I needs to spend a while learning more or working out more.
Thanks for wonderful info I used to be looking for this info for my
mission.
This information is priceless. When can I find out more?
hi!,I love your writing so much! percentage we keep in touch
extra approximately your article on AOL? I need an expert in this house to unravel my problem.
Maybe that is you! Having a look ahead to peer you.
When I originally commented I clicked the “Notify me when new comments are added”
checkbox and now each time a comment is added I get three e-mails
with the same comment. Is there any way you can remove me from that service?
Thank you!
Asking questions are in fact nice thing if you are not understanding something totally, but
this post gives fastidious understanding yet.
Today, while I was at work, my sister stole my apple ipad and tested to
see if it can survive a thirty foot drop, just so she can be a youtube sensation. My
iPad is now destroyed and she has 83 views. I know this is
completely off topic but I had to share it with someone!
If some one desires to be updated with hottest
technologies after that he must be pay a visit this web page and
be up to date everyday.
Quality content is the important to be a focus for the people to visit
the website, that’s what this site is providing.
Heya i’m for the first time here. I came across this board and I find
It truly helpful & it helped me out a lot. I’m hoping to present one thing again and help others such as you helped me.
This is my first time pay a quick visit at here and i am genuinely happy to
read all at alone place.
I’ll right away take hold of your rss feed as I can not to find your e-mail
subscription link or e-newsletter service. Do you have any?
Please let me recognize so that I may subscribe. Thanks.
These are actually enormous ideas in about blogging.
You have touched some pleasant points here. Any way keep up wrinting.
Way cool! Some extremely valid points! I appreciate you writing this
article and also the rest of the website is also really good.
Excellent beat ! I wish to apprentice whilst you amend your website, how could i
subscribe for a blog website? The account aided me a applicable deal.
I have been a little bit acquainted of this your broadcast
provided shiny clear concept
Appreciating the dedication you put into your website and
in depth information you provide. It’s nice to come across
a blog every once in a while that isn’t the same old rehashed information. Excellent read!
I’ve saved your site and I’m adding your RSS feeds to my
Google account.
Howdy I am so excited I found your site, I really found you by error, while I was searching on Aol for something
else, Anyways I am here now and would just like to say kudos for
a remarkable post and a all round thrilling blog (I also love the theme/design), I don’t
have time to read through it all at the minute but I have saved it and also included your RSS
feeds, so when I have time I will be back to read more, Please do keep up the great work.
I always used to read piece of writing in news papers but now
as I am a user of internet therefore from now I am using net for articles or reviews,
thanks to web.
Hello there, just became aware of your blog through Google, and found that it’s really informative.
I’m gonna watch out for brussels. I will be grateful if you
continue this in future. Many people will be benefited from your
writing. Cheers!
Hi there! I could have sworn I’ve been to this website before but after going through some of the posts I realized it’s
new to me. Nonetheless, I’m definitely pleased I came across it and
I’ll be bookmarking it and checking back frequently!
Hey there! I just wanted to ask if you ever have any trouble with hackers?
My last blog (wordpress) was hacked and I ended up losing many months of hard work due to
no back up. Do you have any methods to prevent hackers?
Thanks for sharing your thoughts on zona lendir.
Regards
I’m really impressed with your writing skills and also with the layout on your blog.
Is this a paid theme or did you customize it yourself?
Anyway keep up the excellent quality writing, it
is rare to see a great blog like this one these days.
When I initially commented I clicked the “Notify me when new comments are added” checkbox and now each time a comment is added I get several emails with
the same comment. Is there any way you can remove people from that service?
Thanks!
Hi, i think that i noticed you visited my web site
so i came to go back the choose?.I’m attempting to in finding things to improve my website!I suppose its adequate to make use of
some of your concepts!!
I have fun with, lead to I found exactly what I was taking a look for.
You have ended my 4 day lengthy hunt! God Bless
you man. Have a nice day. Bye
I have read so many posts on the topic of the blogger lovers but this article is really a nice paragraph, keep it up.
I don’t even know how I ended up here, but I thought this post was
good. I don’t know who you are but definitely you are going to a
famous blogger if you are not already 😉 Cheers!
I’m amazed, I have to admit. Seldom do I encounter a blog
that’s both educative and entertaining, and without a doubt,
you’ve hit the nail on the head. The issue is an issue that
not enough people are speaking intelligently about.
I’m very happy I stumbled across this during my hunt for something concerning this.
My programmer is trying to convince me to move to .net from
PHP. I have always disliked the idea because of the costs.
But he’s tryiong none the less. I’ve been using WordPress on a variety of websites for about
a year and am worried about switching to another platform. I have heard good things
about blogengine.net. Is there a way I can transfer all my
wordpress content into it? Any help would be greatly appreciated!
Excellent blog right here! Additionally your site loads up very fast!
What host are you the usage of? Can I get your affiliate hyperlink to your host?
I wish my web site loaded up as quickly as yours lol
These are in fact impressive ideas in concerning blogging.
You have touched some nice points here. Any way keep up wrinting.
Hey! Do you use Twitter? I’d like to follow you if that would be okay.
I’m undoubtedly enjoying your blog and look forward to new updates.
Great post however , I was wanting to know if you could write a litte more on this topic?
I’d be very thankful if you could elaborate a little bit more.
Kudos!
Great blog here! Also your website loads up fast! What host are you using?
Can I get your affiliate link to your host? I wish my website loaded up as fast as
yours lol
It’s an remarkable post in favor of all the online viewers; they will obtain benefit from it I am sure.
A fascinating discussion is worth comment. There’s no doubt that that you should write more about this subject, it might not be a taboo subject but
usually folks don’t discuss such issues. To the next!
Kind regards!!
Hello would you mind letting me know which
hosting company you’re using? I’ve loaded your
blog in 3 different browsers and I must say
this blog loads a lot faster then most. Can you recommend a good internet hosting provider
at a honest price? Cheers, I appreciate it!
Yes! Finally something about 4play.
Does your blog have a contact page? I’m having trouble locating it but, I’d like to send you an email.
I’ve got some ideas for your blog you might be interested in hearing.
Either way, great site and I look forward to seeing it improve over time.
Way cool! Some extremely valid points! I appreciate you penning this article
and the rest of the site is also really good.
I always used to study article in news papers but now
as I am a user of internet therefore from now I am using
net for posts, thanks to web.
First of all I want to say terrific blog! I had a quick question which I’d like to ask if you do not mind.
I was curious to know how you center yourself
and clear your head before writing. I have had trouble
clearing my thoughts in getting my ideas out. I truly do take pleasure
in writing but it just seems like the first 10 to 15 minutes are
generally lost just trying to figure out how to begin. Any ideas or hints?
Kudos!
Hey, I think your blog might be having browser compatibility
issues. When I look at your blog in Opera, it looks fine but when opening in Internet Explorer, it has
some overlapping. I just wanted to give you a quick heads up!
Other then that, very good blog!
Hi, i believe that i saw you visited my website so i came to return the favor?.I am
attempting to to find things to improve my web site!I suppose its
adequate to make use of some of your ideas!!
Wonderful blog! I found it while surfing around on Yahoo News.
Do you have any tips on how to get listed in Yahoo News?
I’ve been trying for a while but I never seem to get there!
Appreciate it
Excellent web site. Plenty of helpful information here. I’m sending it to a few pals ans also sharing in delicious.
And of course, thank you on your effort!
I’m gone to inform my little brother, that he should also
pay a visit this webpage on regular basis to get updated from newest reports.
Hello to every one, the contents existing at this web page are truly
remarkable for people experience, well, keep
up the good work fellows.
Good day very nice blog!! Guy .. Beautiful .. Wonderful .. I’ll bookmark
your website and take the feeds also? I’m happy to find so many helpful info here in the post, we’d like develop more techniques on this regard, thanks
for sharing. . . . . .
Your style is so unique in comparison to other folks I’ve read stuff from.
Thank you for posting when you have the opportunity, Guess I
will just book mark this page.
Everything is very open with a precise clarification of
the issues. It was really informative. Your site is useful.
Thanks for sharing!
Very soon this web site will be famous amid all
blogging viewers, due to it’s pleasant posts
It’s truly very difficult in this busy life to listen news on Television, thus I simply
use world wide web for that reason, and take the latest information.
I love what you guys tend to be up too. Such clever work and reporting!
Keep up the excellent works guys I’ve included you guys to blogroll.
Amazing! This blog looks exactly like my old one! It’s on a entirely different topic but it has
pretty much the same page layout and design. Superb choice of colors!
Your style is very unique in comparison to other folks
I’ve read stuff from. Thank you for posting when you have the opportunity, Guess I’ll just book
mark this site.
Greetings from Carolina! I’m bored to death at work so I
decided to browse your site on my iphone during lunch break.
I love the info you present here and can’t wait to
take a look when I get home. I’m shocked at how quick your blog loaded on my mobile ..
I’m not even using WIFI, just 3G .. Anyways, superb blog!
I’ve been exploring for a bit for any high quality articles
or blog posts on this kind of space . Exploring in Yahoo I finally stumbled upon this web
site. Studying this info So i’m glad to show that I’ve an incredibly just right uncanny feeling I came upon just
what I needed. I so much no doubt will make sure
to do not overlook this web site and give it a look on a continuing basis.
I have been browsing online greater than 3 hours today,
but I by no means found any fascinating article like
yours. It is lovely price enough for me.
Personally, if all website owners and bloggers made good content as you probably did, the web will
likely be much more useful than ever before.
You can definitely see your skills within the work you write.
The sector hopes for more passionate writers such as you who aren’t afraid to mention how they believe.
At all times follow your heart.
I know this web site gives quality dependent articles and
additional information, is there any other web site
which presents such information in quality?
This is my first time pay a visit at here and i am actually happy to read all at one place.
all the time i used to read smaller content which
also clear their motive, and that is also happening with this article which I am
reading now.
I was wondering if you ever thought of changing the page layout of your site?
Its very well written; I love what youve got to say.
But maybe you could a little more in the way of content
so people could connect with it better. Youve
got an awful lot of text for only having one or two pictures.
Maybe you could space it out better?
I am really delighted to read this web site posts which includes plenty of valuable facts, thanks
for providing such data.
I’m not sure why but this web site is loading very slow for me.
Is anyone else having this issue or is it a issue on my end?
I’ll check back later and see if the problem still exists.
Hello! I could have sworn I’ve been to this blog before but after
browsing through some of the post I realized it’s new to
me. Anyways, I’m definitely delighted I found it and I’ll be book-marking and checking
back often!
If you are going for most excellent contents like I do,
simply go to see this web page everyday because it offers quality contents,
thanks
You need to take part in a contest for one of the highest quality websites on the web.
I most certainly will highly recommend this blog!
Pretty great post. I simply stumbled upon your weblog and wanted to say that I have really loved surfing around your blog posts.
After all I will be subscribing to your feed and I hope you write again soon!
Hi, yes this post is genuinely fastidious and I have learned
lot of things from it concerning blogging. thanks.
Thanks for finally writing about > Prevention Of fibromyalgia (fatigue, sleep, memory and mood issues) – Health GadgetsNG < Loved it!
Its such as you learn my mind! You appear to understand so much about this,
such as you wrote the ebook in it or something.
I feel that you simply could do with some % to force the message house a bit,
but instead of that, that is excellent blog. A great read.
I will certainly be back.
Hi, I check your new stuff like every week. Your humoristic style
is awesome, keep doing what you’re doing!
Way cool! Some very valid points! I appreciate you penning this post plus the rest of the site is really good.
I just could not leave your site prior to suggesting that I really enjoyed the standard information a person provide
on your visitors? Is going to be again continuously in order to
inspect new posts
After looking at a handful of the articles on your web site,
I really like your technique of blogging.
I saved as a favorite it to my bookmark website list and
will be checking back soon. Take a look at my web site too and tell me
how you feel.
When I initially commented I clicked the “Notify me when new comments are added” checkbox and now
each time a comment is added I get three e-mails with
the same comment. Is there any way you can remove people from that service?
Thank you!
Do you mind if I quote a couple of your articles
as long as I provide credit and sources back to your website?
My blog is in the very same area of interest as yours and my visitors would genuinely benefit
from some of the information you present here.
Please let me know if this ok with you. Cheers!
Good article. I absolutely love this website. Keep it up!
Everything is very open with a very clear explanation of the challenges.
It was truly informative. Your site is extremely helpful.
Many thanks for sharing!
My family members always say that I am wasting my time here at web, but I know I
am getting experience every day by reading such good
posts.
jermell cobano
It’s genuinely very complicated in this busy life to listen news on TV, so I just
use internet for that purpose, and take the latest news.
Also visit my homepage … vpn coupon 2024
Greate post. Keep writing such kind of information on your blog.
Im really impressed by your site.
Hey there, You have performed a great job. I will certainly digg it and in my opinion suggest to my friends.
I’m confident they’ll be benefited from this web site.
Feel free to surf to my website vpn special coupon code 2024
п»їlegitimate online pharmacies india https://indiaph24.store/# top 10 online pharmacy in india
Online medicine home delivery